Individual and group therapy differ in five key ways: customized treatment versus shared experiences, privacy levels, cost ($50-150 vs. $15-35 per session), professional guidance versus peer support dynamics, and comprehensive therapeutic approach. You’ll find individual sessions offer personalized attention and maximum confidentiality, while group settings provide community connection and cost savings. The best choice depends on your specific diagnosis, comfort with disclosure, and practical considerations. Understanding these distinctions will help you make an informed decision about your mental health care.
The Personal Touch vs. Community Connection
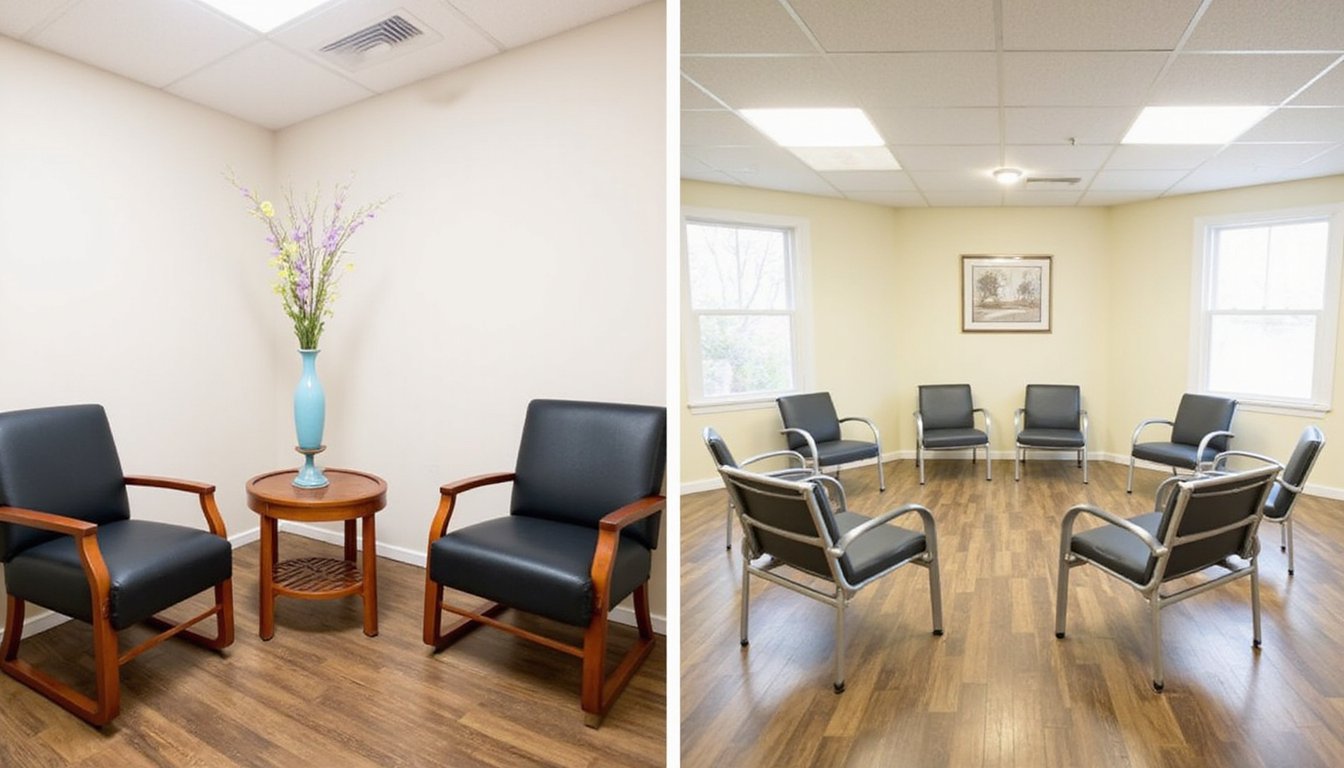
Every individual seeking mental health treatment faces a fundamental choice between two distinct therapeutic environments. When you choose individual therapy, you’ll receive customized treatment plans adapted exclusively to your needs, allowing for in-depth processing of personal challenges in a private setting. Your therapist can provide immediate, focused feedback on your specific situation and progress. Most individual sessions last 45-60 minutes, allowing for concentrated therapeutic work.
Group therapy, however, offers unique advantages through shared experiences and mutual understanding. You’ll find yourself part of a supportive community where you can develop social skills and learn from others’ coping strategies. Research shows that group settings can cultivate essential psychological qualities like sense of belonging and hope. While individual therapy provides concentrated one-on-one attention, group settings create opportunities for interpersonal learning and collective growth. Research shows both approaches effectively reduce symptoms, though individual therapy typically has lower dropout rates and initially receives more favorable ratings from patients.
Confidentiality and Comfort Levels Matter
When choosing between individual and group therapy, confidentiality and personal comfort greatly influence treatment effectiveness and outcomes. Individual therapy offers the highest level of privacy, with only you and your therapist privy to session content. This controlled environment often creates a more supportive environment for discussing sensitive issues. Experienced therapists assess each client’s unique circumstances to recommend the most appropriate format based on their privacy needs. Group therapy, while beneficial in many ways, presents unique privacy concerns since confidentiality depends on all participants’ commitment to discretion. You’ll find that comfort levels typically start lower in group settings due to peer presence but may increase as trust develops among members. The emphasis on personal exploration helps clients work through vulnerability concerns at their own pace. Your therapist is legally and ethically bound to protect confidentiality in both formats, though absolute privacy can’t be guaranteed in group sessions. Patient autonomy is prioritized when discussing privacy concerns during the informed consent process. Consider your personal need for privacy and comfort when selecting the most appropriate therapeutic approach.
Cost Considerations and Treatment Access

Beyond privacy concerns, financial factors meaningfully shape therapy choices. You’ll find individual therapy typically costs $50-$150 per session in developed nations, while group therapy runs $15-$35, a 60-80% reduction. Your location drastically impacts these rates, with provider scarcity in rural areas often driving up costs despite lower costs of living. In states like South and North Dakota where there is only one psychologist per 5000 residents, therapy costs are among the highest nationwide.
Insurance coverage varies widely for both formats, though group sessions usually carry lower copays. Recent research shows that group therapy can produce a cost savings threshold of $141 per reduced drinking day compared to individual therapy. While specialized offerings may cost more, they can deliver targeted value for specific conditions. Your out-of-pocket expenses depend heavily on insurance status, with cash rates averaging $167.69 versus lower contracted insurance rates. Despite the higher cost of individual sessions, both formats prove clinically effective, making group therapy a particularly cost-efficient option when appropriate for your needs. Studies show that participants receiving group therapy experienced meaningful improvement in depression symptoms.
Peer Support vs. Professional Guidance
Both peer support and professional guidance serve distinct yet complementary roles in mental health treatment. While peer support capitalizes on shared experiences and informal self-disclosure patterns, professional therapy follows structured clinical protocols aimed at measurable outcomes. Research shows both approaches can effectively reduce depression and anxiety symptoms, though through different mechanisms. Peer supporters occupy a unique position as they work within the liminal space between patient and clinician roles. Peer support platforms provide trained listeners online who can offer basic emotional guidance while directing users to professional help when needed. Psychotherapy groups are characterized by their formal structure and require licensed therapists to maintain therapeutic frameworks.
Key distinctions between these approaches include:
- Peer support emphasizes mutual understanding and community connection through lived experience sharing
- Professional guidance focuses on evidence-based interventions and standardized therapeutic techniques
- Peer support allows flexible, participant-driven discussions without formal clinical oversight
- Professional therapy requires licensed clinicians who maintain clear boundaries and monitor specific treatment goals
You might benefit from combining both approaches, using professional therapy for clinical needs while accessing peer support for ongoing community and validation.
Finding Your Best Therapeutic Match

How do you determine which therapy format will best serve your mental health needs? Research shows both individual and group therapy yield comparable outcomes for most conditions, but treatment suitability depends on several key factors.
Consider your diagnosis and symptom specificity, group therapy often works better for focused issues like substance use or chronic pain, while individual therapy may be preferable for complex trauma or severe psychiatric symptoms. Your personality and comfort with disclosure matter too. If you’re highly antisocial, extremely shy, or struggle with impulse control, individual sessions might be more beneficial.
Practical considerations should also guide your choice. While group therapy costs less and offers peer support, individual therapy provides more scheduling flexibility and personalized attention. Your cultural background and language needs may influence which format better serves your therapeutic goals.
Frequently Asked Questions
How Long Does Each Type of Therapy Session Typically Last?
You’ll find that individual therapy sessions typically last 45-60 minutes, while group therapy sessions run longer at 60-90 minutes. Session frequency is usually weekly for both formats, though you might schedule individual sessions biweekly depending on your needs. Research shows the average session duration is 60 minutes for individual therapy and 90 minutes for group sessions. These timeframes allow for adequate therapeutic work while maintaining consistent scheduling patterns.
Can Someone Switch Between Individual and Group Therapy During Treatment?
Yes, you can switch between individual and group therapy during your treatment. Most mental health providers offer therapy modality flexibility to accommodate your changing needs and goals. You’ll find smooth shifts between individual and group formats are common and often advantageous. Your therapist may recommend switching based on your progress, or you can request a change. Many treatment plans even combine both modalities simultaneously for extensive care and ideal results.
What Qualifications Should Therapists Have for Group Versus Individual Sessions?
You’ll find that therapists leading both individual and group sessions must have core mental health licensure (PhD, LCSW, LPC, or MD). For group therapy, they need supplementary specialized training requirements in group dynamics and supervised group facilitation experience. While individual therapy focuses on one-on-one clinical skills, group leaders must master unique competencies like managing multiple relationships, fostering group cohesion, and ensuring balanced participation among members.
How Many Participants Are Usually Included in Group Therapy Sessions?
You’ll typically find 6-12 participants in group therapy sessions, with most experts considering 7 members the best group size. Group size variations depend on several factors, including therapy type, setting, and patient population. For preferred outcomes, therapists maintain specific therapist-patient ratios, usually 1-2 therapists per group. While smaller groups (4-5 members) allow more individual attention, larger groups (up to 12) offer diverse perspectives but may limit participation opportunities.
Are Virtual Options Available for Both Individual and Group Therapy?
Yes, you’ll find virtual options readily available for both individual and group therapy through diverse platforms. Research confirms that online therapy accessibility has expanded considerably, offering comparable treatment outcomes to in-person care. Virtual session quality matches traditional therapy for conditions like anxiety and depression in both formats. You can access these services through telehealth providers, private practitioners, and specialized mental health apps, all offering secure, HIPAA-compliant environments.





